What Sudden Spikes in HIV Viral Load Really Mean
 November 5, 2008
November 5, 2008 The following was written by Professor John Mills, Monash University, Australia, who I have had the pleasure to work with for a number of years. John is an authority in the HIV field, having extensive experience both in research and in practice, including measuring viral load with our ExaVir Load assay. I’m posting this piece because it does a great job of explaining what HIV viral load blips are, when you should be worried and when it’s a false alarm.
An elevated HIV viral load on therapy: is it a "blip" or a "bust"?
Although measurements of HIV viral load are useful for assessing the prognosis and need for treatment of patients not on anti-retroviral therapy (ART), they are absolutely critical for monitoring the efficacy of therapy.
When treatment naïve patients are started on combination ART, the HIV viral load should fall very quickly. Usually within 2-3 months, and certainly by 3-6 months, the viral load should be "undetectable".
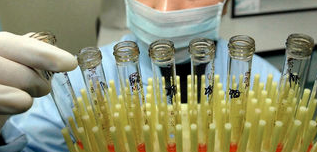 What constitutes an "undetectable" viral load depends on the assay system used. It varies from less than 400 copies/ml to less than 40 copies/ml. Although it might seem that <40 is better than <400, to date the evidence suggests they are equivalent. Clearly, however, viral loads at or above 400 are a real cause for worry (Pilcher et al, 1999).
What constitutes an "undetectable" viral load depends on the assay system used. It varies from less than 400 copies/ml to less than 40 copies/ml. Although it might seem that <40 is better than <400, to date the evidence suggests they are equivalent. Clearly, however, viral loads at or above 400 are a real cause for worry (Pilcher et al, 1999).
Once a patient on ART achieves an "undetectable" viral load, it should remain undetectable indefinitely if they continue to take their ART as directed, and do not develop an unusual circumstance that would interfere with drug efficacy (e.g. drug interactions or a gastrointestinal condition interfering with drug absorption or metabolism).
Surprisingly, a number of studies, including ones in which viral loads were measured daily (Nettles et al, 2005) – as well as substantial clinical experience – have shown that many patients will have transient elevations of viral load known as "blips." Blips are defined as transient, low-level increases in viral load. Specifically, they are a single detectable HIV viral load measurement of less than 1000 (although rare blips may be slightly higher than that), which is immediately preceded and followed by an undetectable viral load (Gallant 2007).
Argument continues as to whether blips are a laboratory artifact or represent true HIV viremia. I think the weight of evidence is that they do represent short-term viremia.
In an individual patient, the frequency of blips seem to be related to less than perfect adherence to the treatment regimen – patients who have missed ART doses in the week prior to the blip are more likely to have them than patients who are highly adherent (Podsadecki et al, 2007). Curiously, however, blips do not seem to predict subsequent development of an HIV strain resistant to ART ("virologic failure" of the ART regimen).
How can you tell if a patient who previously has had an undetectable viral load has just a "blip", or whether it is a "bust" – an elevated viral load likely indicating that the ART regimen is failing (due to resistance, poor adherence, poor absorption or drug interactions)?
If the renegade viral load is well above 1000, it is almost certainly a "bust." But the only way to definitively answer the "Blip or Bust" question is to perform another viral load assay, ideally 3-8 weeks later than the first. Even if the first value is well above 1000, it could still represent a lab error and should be repeated (you wouldn't want to switch a patient to a second line regimen on the basis of an erroneous viral load!).
If the first viral load value is >1000, and the second value is also >1000, and especially if it is higher than the first, it is almost certainly a "bust", and the patient should be investigated for ART regimen failure.
If the first value is <1000, and the second value is back to undetectable, you can relax as you're seeing a blip. However, since blips are related to episodic lapses of adherence, it is definitely worth reminding the patient that the best results from ART are achieved if 100% of doses are taken.
References
Gallant JE (2007). Making sense of blips. J Infect Dis, 196:1729-31
Nettles RE, Kieffer TL, Kwon P, et al. (2005). Intermittent HIV-1 viremia (blips) and drug resistance in patients receiving HAART. JAMA 293: 817-829.
Pilcher CD, Miller WC, Beatty ZA, Eron JJ. (1999). Detectable HIV-1 RNA at levels below auntifiable limits by Amplicor HIV Monitor is associated with virologic relapse on antiretroviral therapy. AIDS 13:1337-42.
Podsadecki TJ, Vrijens BC, Tousset EP et al. (2007). Decreased adherence to antiretroviral therapy observed prior to transient human immunodeficiency virus type 1 viremia. J Infect Dis 196:1773-8.

Reader Comments (16)
thanks!!!